A cycling accident. The loss of a beloved grandmother. A career-ending sports injury. These University of Florida researchers are united by deeply personal experiences that motivate them to understand the brain — and make it work better amid disease or injury.
Mapping the brain—and a path back from her own injury
Even after years of studying deep brain stimulation, what fascinates Aysegul Gunduz the most is the brain’s ability to adapt — to allow artificial electrical current to alter cell activity and quell tremors or tics, seizures or involuntary muscle contractions.
“People say you can’t teach an old dog new tricks, but you really can,” says Gunduz, a biomedical engineer and director of UF’s Brain Mapping Laboratory.
Three and a half years ago, her longstanding appreciation of the brain’s plasticity was put to the test: She herself was wheeled in under the bright lights, her brain the one to be operated on.
She had been training for a triathlon on a new bicycle when she suddenly hit a rough patch of pavement, lost control and fell. Although she was wearing a helmet, the impact caused a traumatic brain injury and a need for emergency surgery to relieve pressure in her head and stop seizures.
Dr. Brian Hoh, chair of UF neurosurgery, performed the operation. The days before and after were a blur to her, but one thing she knew in her heart, she says: “I owe him my life.”
Every day in intensive care, she was visited by her longtime collaborators Dr. Michael Okun, a neurologist, and Dr. Kelly Foote, a neurosurgeon. A decade earlier, Okun and Foote, now co-directors of the Fixel Institute, had been searching for an expert who could analyze brain signals in their pursuit of continuing to improve deep brain stimulation for Parkinson’s disease and other conditions. They’d been working as a team ever since.
“She is creative, she is innovative, and she is brilliant,” Okun says. “She’s an expert at taking the language of the brain and converting it into units that we can use to decode certain symptoms and develop therapies.”
Gunduz sensed quickly it was the right fit. “Sometimes clinicians think engineers are like technicians who magically put together the things they want,” she says with a chuckle. “But Mike and Kelly gave me an equal seat at the table. They lift up people around them.”
Years later, as she healed from the accident, support and encouragement from many — her fiancé (now husband), colleagues and family back in Turkey — helped her get back on track. Care by UF neuropsychologist Russell Bauer, an expert in traumatic brain injury, and the UF Health rehab team helped her get back to work and fueled her determination.
Over time, her perspective on the accident has evolved. “As ironic as it is for this to happen to a brain researcher, I knew my brain could regain the functions that were impaired,” says Gunduz, whose many awards over the years include the Gator Nation Leadership Award and the Presidential Early Career Award for Scientists and Engineers, the highest honor given by the U.S. government to outstanding scientists and engineers beginning independent careers.

“Having worked with a lot of neurosurgical patients, I knew that if you keep at it, your brain can heal itself,” she says. “So that kept me going, as well as the promise I had to my Ph.D. students. And my father is a physical medicine rehabilitation doctor back in Turkey, so that kept me going, too.”
All along, she held onto a deep belief in her capacity to grow, a belief that stretched back to her school days, when a teacher once told her, “I don’t see you becoming an engineer.” After initial tears, she didn’t give up, and in summer 2023 she shared the teacher’s words on social media on the day she was promoted to full professor of biomedical engineering.
Her determination to recover from the accident and get back to her research was no surprise to longtime colleagues such as Peter Brunner, who worked with Gunduz during her postdoctoral fellowship at Albany Medical College in 2011.
“She not only made a remarkable recovery, but she also has gained extremely valuable insight for herself on how the human brain is plastic and how it can recover,” says Brunner, an associate professor of neurosurgery and biomedical engineering at Washington University in St. Louis. “This is really a compliment to all the physicians involved in her recovery but also to her perseverance and strong push to move forward.”
Not only did she make it through, he says, but “she came back out on the other side even stronger.”
Brunner saw the same spark in her at the start of her career, when she chose to pursue a line of technological research considered risky at the time: detecting debilitating tics, which then was seen as the cutting edge of what scientists thought could be done.
“She picked something that’s really difficult and literally bet the farm on it,” Brunner says. “She picked something nobody really saw taking off and was extremely successful and developed herself into one of the world experts in deep brain stimulation.”
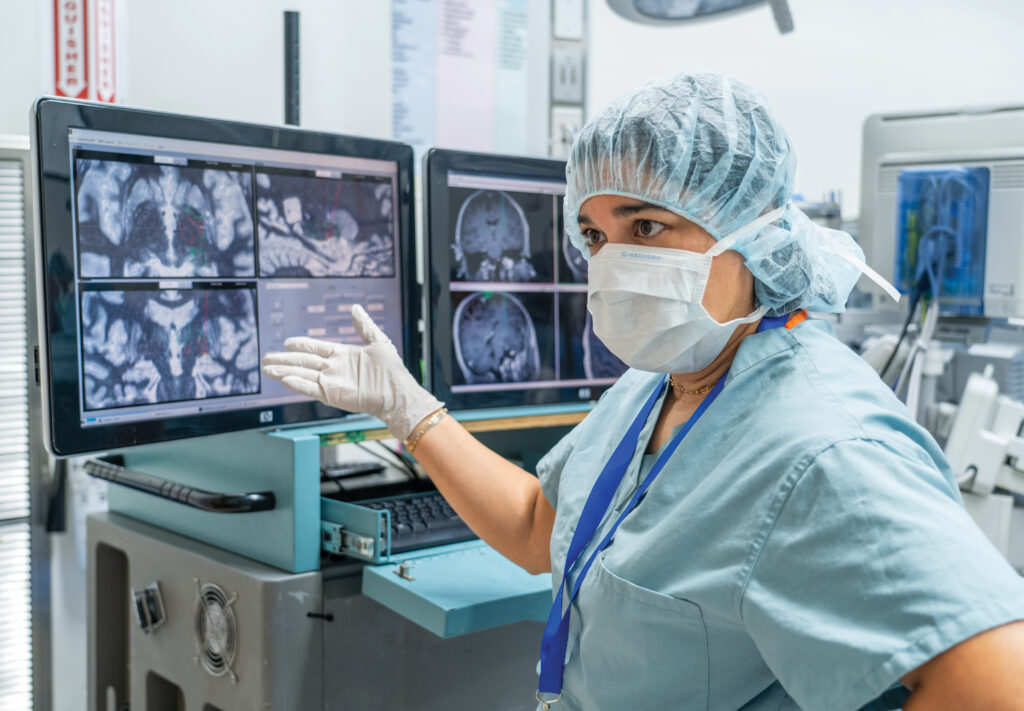
Today, Gunduz, the inaugural Fixel Brain Mapping Professor, is back in the operating room at the UF Health Neuromedicine Hospital. With MRI images on a monitor beside her, she watches as innovative software she developed is used in patients undergoing deep brain stimulation (DBS) surgery to ease symptoms in conditions including Tourette syndrome and essential tremor.
Her current focus is to make DBS more like a cardiac pacemaker, in a way — to make the mild pulses of electricity responsive to changing signals in the brain rather than continuous, to limit side effects and the draining of the implant’s battery.
Some days in the operating room, the team uses software she developed to map the brain of a patient to guide implantation of an electrode. Other days, she is collecting neurophysiological data, for later decoding of brain signals to refine aspects of DBS and develop the next generation of software.
“She is guiding the future,” says Okun, “of how the brain is going to be targeted and how we’re going to intervene.”

